From Lewis S Blevins Jr, MD – Pituitary cysts come in a variety of different sizes and flavors.
Before we talk about them it is useful to review pituitary embryology. The pituitary gland develops from a flat piece of the upper mouth and back of the nose of the embryo. This tissue grows upwards and pouches out forming the Rathke’s pouch. This ultimately pinches off forming a ball of cells and migrates into the future location of the sella turcica. Cells that reside in the ball start expanding, asymmetrically, forming the anterior pituitary gland. The cavity that started out in the middle of this group of cells usually gets obliterated. The thinner part of the ball of cells usually dies. In some species this persists as what is known as the pars intermedia or intermediate lobe of the pituitary gland. The posterior pituitary goes down from the brain from the anterior pituitary. The space between them, which is also adjacent to the obliterated cavity, is actually a tissue plane. In this region is located an occasional embryologic remnant of the part of the pituitary that came from the upper mouth known as the Rathke’s cleft. This cleft is best seen on histologic sections through the anterior and posterior pituitary gland. Sometimes, we see it on the MRI of the pituitary gland.
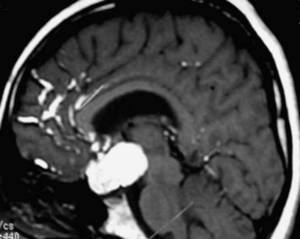
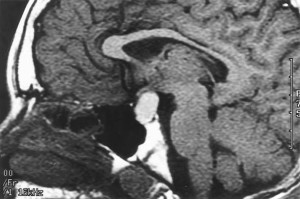
Occasionally, a little tiny cyst can be formed in the location of the Rathke’s cleft or the area where the pars intermedia was to be located if it persisted. These are known as pars intermedia cysts. They’re usually 1-3 mm in size. We usually presume they have been present since birth. In over a quarter century I have not seen a single one of these increase in size but we recommend followup MRI in about 2-3 years if one is Identified just in case the lesion represents an early Rathke’s cleft cyst.
Rathke’s cleft cysts are usually larger. There are also more distinct. They do increase in size with time. They may represent a pars intermedia cyst that decides to increase in size over time. No one knows for sure. Obviously, they started out small at some point and then enlarged with time. These cysts have a single simple cuboidal cell lining. The cells in the cyst believe that it is their job to make fluid. They store that fluid within the cyst. Think of these as self-filling water balloons of the pituitary gland. They can cause problems in that some patients will have headaches while others will have dysfunction of the pituitary gland due to mass effect of the cyst on the normal anterior gland. Generally speaking, surgery is indicated if A Rathke’s cleft cyst causes pituitary dysfunction, headaches, or demonstrates an increase in size, extends into the suprasellar cistern causing visual compromise, or is greater than 1 cm in dimension. Occasionally, Rathke’s cleft cysts can be infected. If so, the recurrence rate is much higher than the usual recurrence rate of about 8-12%. Some people are said to have pituitary abscesses when, in fact, what they had was an infected Rathke’s cleft cyst.
Arachnoid cysts are in invagination of the arachnoid membrane, that usually lines the skull cavity, into the sella or suprasellar region. Somehow, If the cyst has a fold and it came close off an opening, there is the the possibility of accumulation a collection of spinal fluid within this cyst. The real problem with these is that fluid gets and cannot get out. They simply accumulate fluid over time and increase in size. The cyst lining itself does not make fluid. They are usually slow-growing and are rather large before pituitary dysfunction becomes. Most are in the suprasellar region. They do require surgery on occasion When there are headaches or hypopituitarism or other mass effects due to these lesions
The empty sella syndrome as a form of an arachnoid invagination and spinal fluid located within the sella but the fluid in the sella communicates with the fluid around the brain. The empty sella syndrome has been discussed elsewhere on our pages. Surgery is usually not required for this particular disorder.
Epidermoid cysts are rare but can occur in and around the region of the pituitary gland and suprasellar cistern. These are basically embryologic rests of skin cells the former cyst and make all sorts of skin related gunk that can collect within them. For example, keratin , which is the outer layer of skin, accumulates within them. Some have teeth or hair. They can occasionally rupture into the spinal fluid and cause a sterile meningitis. They’re very difficult to treat and often recur after surgery. This lesion requires a most excellent Pituitary surgeon to address correctly and decrease the likelihood of future problems.
Neurocystercosis is a very rare disorder that can present with cysts in the region of the pituitary stalk and hypothalamus. These cysts usually occur in other areas of the brain as well. Basically, this is a tapeworm Infestation of the central nervous system. The nematodal cysts of the tapeworm mimic other cystic diseases of brain. I have seen a couple of patients with this disorder. They presented with hyperprolactinemia, partial hypopituitarism, and suprasellar cysts. Most of my patients had a history of travel to Mexico or having eaten under cooked pork.
Of course, this post does not address cystic pituitary adenomas and cystic craniopharyngiomas. These lesions are usually very readily differentiated from the cysts mentioned above except some of the epidermoid cysts do mimic craniopharyngioma.
An epidermoid cyst with rupture of contents into the spinal fluid showing up as the white patchy areas in the region of the frontal lobe of the brain.
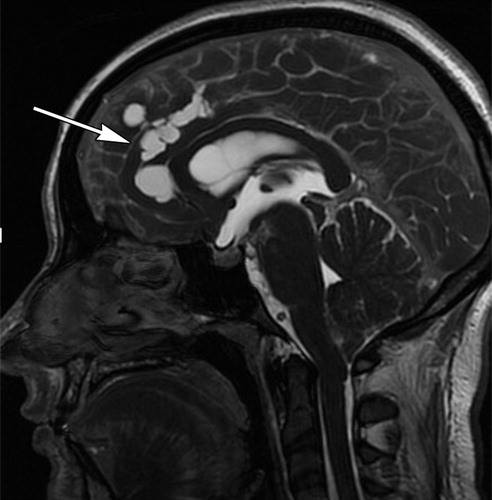 Neurocysticercosis with multiple cystic areas in the brain
Neurocysticercosis with multiple cystic areas in the brain
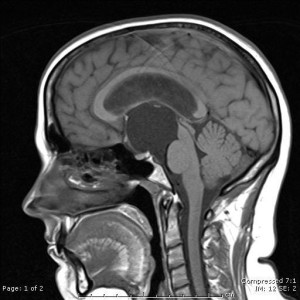 A rather large suprasellar arachnoid cyst
A rather large suprasellar arachnoid cyst
© 2015 – 2016, Pituitary World News. All rights reserved.